Custom Orthotics Seasonal - Any Season

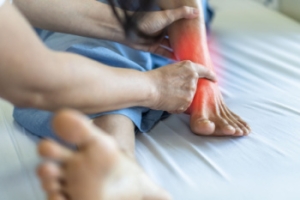
Rain or shine, snow or sleet, Custom Orthotics have your feet covered! As the seasons change, ensure your steps remain comfortable and supported. Custom Orthotics adapt to your footwear, from summer sandals to winter boots, providing consistent relief and alignment. Don't let the changing weather dictate your foot comfort. Step confidently year-round and experience the difference with Custom Orthotics. Call today for more information.
Managing Plantar Fasciitis

Plantar fasciitis is a common cause of heel pain, typically felt as a sharp or stabbing sensation, especially with the first steps in the morning or after long periods of sitting. The pain is caused by inflammation of the plantar fascia, a thick band of tissue that connects your heel to your toes. Overuse, flat feet, high arches, or wearing unsupportive footwear can increase your risk of developing this condition. In addition to heel pain, you may also experience tightness or swelling along the bottom of the foot. Treatments often include rest, stretching exercises, and wearing supportive shoes or custom orthotics to relieve pressure. In more severe cases, a podiatrist may recommend corticosteroid injections or even surgery. This type of specializes in diagnosing and treating conditions like plantar fasciitis, and they can tailor a treatment plan to help alleviate pain and prevent future flare-ups. If you are struggling with heel pain, it is suggested that you schedule an appointment with a podiatrist for effective treatment solutions.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact one of our podiatrists from BayCity Associates in Podiatry . Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions, please feel free to contact our offices located in Erie, PA and Meadville, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Relief for Bunion Pain With Orthotics

Custom orthotics can be a powerful tool in managing bunion pain, especially when paired with properly fitted shoes. Bunions develop from misaligned joints at the base of the big toe, causing discomfort, swelling, and difficulty with footwear. Orthotics help by redistributing pressure away from the bunion, reducing friction and inflammation. They also improve foot alignment, which minimizes the progression of the bunion over time. When worn in supportive, roomy shoes that do not compress the toes, custom orthotics provide optimal relief. Look for shoes with a wide toe box and cushioning to complement the benefits of the orthotics. Together, they help alleviate pain and allow for more comfortable daily activities. While orthotics will not reverse bunions, they can significantly improve quality of life. If you have a painful bunion, it is suggested that you see a podiatrist for expert advice and care.
Custom orthotics are specialized shoe inserts created to support and align the feet according to each person’s unique structure and walking pattern. They are an effective way to relieve foot discomfort caused by conditions such as flat feet, high arches, plantar fasciitis, bunions, and heel pain. When the natural alignment of the foot is off balance, it can lead to pressure points, strain, and pain that affect how a person stands, walks, and moves. Orthotics work by redistributing weight evenly and supporting the arch to reduce stress on the muscles, tendons, and joints of the feet and lower legs.
Foot discomfort can develop for many reasons, including wearing improper footwear, long hours of standing, repetitive motion, or underlying structural problems. Over time, this discomfort can extend beyond the feet, contributing to knee, hip, or lower back pain. Custom orthotics help correct these issues by improving alignment and promoting more efficient movement. They are made using precise measurements and imaging to ensure the best fit for each patient, providing targeted support and cushioning where it is needed most.
Unlike generic insoles, custom orthotics are durable, medically designed, and tailored to your specific needs. Whether you are managing chronic pain, recovering from an injury, or simply seeking better comfort and stability, orthotics can make a noticeable difference in how your feet feel throughout the day.
If you are experiencing persistent foot discomfort or fatigue, it may be time to have your feet evaluated by a podiatrist. Call our office today for more information or to schedule an appointment.
If you have any questions, please feel free to contact our offices located in Erie, PA and Meadville, PA .
Investing in Custom Orthotics Means Investing in Foot Health
Custom orthotics offer a tailored approach to foot health, providing a host of benefits that extend far beyond conventional shoe inserts. One of the primary advantages lies in their ability to address specific biomechanical issues. Unlike off-the-shelf inserts, custom orthotics are crafted based on an individual's unique foot structure, gait, and any existing foot conditions.
The personalized design of custom orthotics ensures optimal support for the arches, promoting proper alignment and distributing pressure evenly across the feet. This can be particularly beneficial for individuals dealing with issues such as overpronation or underpronation, as custom orthotics help correct imbalances that may lead to discomfort or injury.
Beyond biomechanics, custom orthotics can alleviate a range of foot problems, including plantar fasciitis, bunions, and metatarsalgia. They provide targeted relief to areas under stress, reducing pain and inflammation. Additionally, for those with specific medical conditions like diabetes, custom orthotics can play a crucial role in preventing complications associated with poor foot health.
Comfort is another key aspect of custom orthotics. By accommodating the unique contours of an individual's feet, these inserts enhance overall comfort, making daily activities more enjoyable. Whether for athletes looking to optimize performance or individuals seeking relief from chronic foot pain, custom orthotics offer a versatile solution.
Investing in custom orthotics is an investment in long-term foot health. They not only provide immediate relief but also contribute to the prevention of future issues. With the ability to seamlessly integrate into various types of footwear, custom orthotics empower individuals to prioritize foot comfort without compromising on style. In essence, custom orthotics are a personalized prescription for happy, healthy, and pain-free feet.
Surgery for Tarsal Tunnel Syndrome
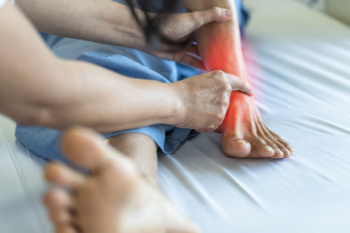
Tarsal tunnel syndrome happens when the tibial nerve is compressed inside the tarsal tunnel, a narrow space in the ankle. It causes tingling, burning, numbness, or sharp pain in the foot, often worsening with activity. People with flat feet, diabetes, arthritis, or previous ankle injuries are more likely to develop it. Doctors diagnose tarsal tunnel syndrome with a physical exam, nerve conduction tests, and sometimes imaging like an MRI scan. When conservative treatments like rest, orthotics, and targeted exercises do not help, surgery may be an option. Tarsal tunnel release surgery involves cutting the ligament over the nerve to relieve pressure. This can reduce pain and prevent further nerve damage. Recovery and satisfaction with the surgery varies, but exercises may help restore strength and movement. If you have persistent foot pain or numbness, it is suggested that you see a podiatrist for a proper diagnosis and treatment.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact one of our podiatrists of BayCity Associates in Podiatry . Our doctors can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please contact our offices located in Erie, PA and Meadville, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
Managing an Ingrown Toenail

An ingrown toenail occurs when the edge of a toenail grows into the surrounding skin, causing pain, swelling, and redness. This condition commonly affects the big toe and can be caused by improper nail trimming, wearing tight shoes, or injury. People with naturally curved nails or certain foot conditions are more prone to developing ingrown toenails. Symptoms include sharp pain, swelling, redness, and in some cases, the formation of pus if an infection develops. The area surrounding the nail may feel tender or sore, especially when walking or wearing shoes. Treatment for an ingrown toenail starts with soaking the foot in warm water to reduce swelling. For mild cases, a podiatrist may lift the nail or trim it carefully. In more severe cases, part of the nail may need to be removed or treated with a local anesthetic. If you are experiencing an ingrown toenail, it is suggested that you schedule an appointment with a podiatrist for proper care.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact one of our podiatrists of BayCity Associates in Podiatry . Our doctors can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions, please feel free to contact our offices located in Erie, PA and Meadville, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ingrown Toenail Care
An ingrown toenail is a toenail that grows sideways into the nail bed, causing pain and swelling. Ingrown toenails can worsen and cause drainage, turning into a serious infection.
Several factors affect whether a person is at risk from an ingrown toenail. The many causes include being overweight, diabetes, participating in sports, having a fungal infection of the toe, and cutting your nails too short. Ingrown toenails also have a genetic predisposition, causing some people to be more prone to receive the condition than others. Other causes include improperly fitting shoes and shoes that keep the feet damp.
Ingrown toenails can be preventable with certain measures. For starters, allowing your toe nails to grow slightly longer in length will help prevent them from becoming ingrown. If you have already developed an ingrown toenail, soak the affected toe in warm water. This will alleviate the pain and help prevent an infection from forming. Antibiotic soap or Epsom salts may be added to further help the relieving process and avoid infection. Placing cotton beneath the affected area is also suggested, as this may help the toenail grow upwards and not into the nail bed. Swelling and redness can be reduced by resting with your feet elevated.
A podiatrist should be seen if the pain becomes so serious that it prevents you from doing your everyday activities. If a red streak running up your leg appears or if you suspect your infection has spread, contact a podiatrist immediately. Fast treatments can be undertaken to lessen your pain and have you walking comfortably.
An ingrown toenail can be easily treated with a Band-Aid. Simply wrap the affected toe with a Band-Aid to prevent infection and keep the nail from growing out at a painful angle.
In more serious cases, your podiatrist may decide to make a small incision to remove a portion of your toenail. To prevent the nail from growing back, medication will be placed directly into the nail bed. This procedure would be performed under local anesthesia and is a faster method to alleviate discomfort from an ingrown toenail. Post-procedure directions will have you stay off the affected foot for a day. Afterwards, normal activities can be resumed.